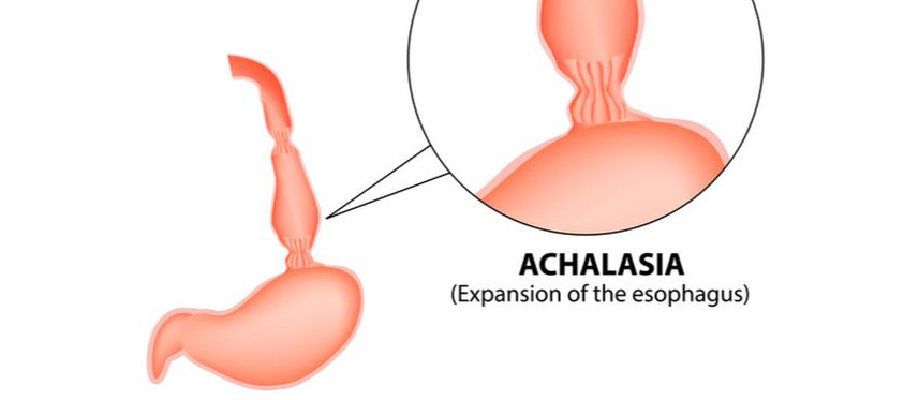
Achalasia cardia is a rare but serious swallowing disorder that affects the food pipe (esophagus). In this condition, the lower end of the esophagus fails to relax properly, making it difficult for food and liquids to pass into the stomach. Over time, this can cause significant discomfort, weight loss, and nutritional problems. Laparoscopic Achalasia Cardia Surgery is a minimally invasive and effective treatment option that provides long-term relief from symptoms.
This article covers everything a patient needs to know about laparoscopic treatment for achalasia cardia, including causes, symptoms, diagnosis, treatment options, procedure details, recovery, and risks.
What Is Achalasia Cardia?
Achalasia cardia is a disorder in which the muscles of the esophagus do not work properly. The lower esophageal sphincter (LES), which normally opens to allow food into the stomach, remains tightly closed. Additionally, the normal wave-like movements of the esophagus (peristalsis) are absent.
As a result, food gets stuck in the esophagus instead of passing smoothly into the stomach.
Causes of Achalasia Cardia
The exact cause of achalasia is not fully understood. It is believed to occur due to damage to the nerves that control the esophageal muscles. Possible contributing factors include:
- Autoimmune reactions
- Viral infections
- Genetic factors
- Degeneration of esophageal nerves
Achalasia is not caused by diet or lifestyle and can occur at any age.
Symptoms of Achalasia Cardia
Symptoms usually develop gradually and may worsen over time. Common symptoms include:
- Difficulty swallowing solids and liquids
- Regurgitation of undigested food
- Chest pain or discomfort
- Heartburn-like symptoms
- Weight loss
- Chronic cough or aspiration at night
- Recurrent chest infections
Diagnosis of Achalasia Cardia
To confirm the diagnosis, doctors may recommend:
- Barium swallow X-ray to assess esophageal shape and emptying
- Upper GI endoscopy to rule out other conditions
- Esophageal manometry, the gold standard test to measure muscle pressure
- CT scan in selected cases
Treatment Options for Achalasia Cardia
Treatment aims to relax the lower esophageal sphincter and improve food passage. Options include:
- Medications (limited benefit)
- Endoscopic balloon dilatation
- Botox injections (temporary relief)
- Laparoscopic Heller's Myotomy with Fundoplication (most effective long-term solution)
What Is Laparoscopic Achalasia Cardia Surgery?
The standard surgical treatment for achalasia is Laparoscopic Heller's Myotomy. This minimally invasive procedure involves cutting the tight muscles of the lower esophagus to allow easier swallowing. To prevent acid reflux after surgery, a partial fundoplication (wrapping part of the stomach around the esophagus) is usually performed.
Benefits of Laparoscopic Surgery
Compared to open surgery, laparoscopic treatment offers:
- Small incisions and minimal scarring
- Less postoperative pain
- Short hospital stay
- Faster recovery
- Long-lasting symptom relief
- Improved quality of life
Preparation Before Surgery
Before surgery, patients may be advised to:
- Undergo blood tests and imaging
- Follow a liquid diet for a few days
- Fast for 6–8 hours before surgery
- Attend pre-anesthesia evaluation
- Stop smoking if applicable
What Happens During the Procedure?
The surgery is performed under general anesthesia and usually involves:
- Making 4–5 small abdominal incisions.
- Inserting a laparoscope for visualization.
- Cutting the tight muscle fibers of the lower esophagus and upper stomach.
- Performing partial fundoplication to reduce reflux.
- Closing the incisions.
The procedure typically takes 1.5 to 2.5 hours.
Recovery After Laparoscopic Achalasia Surgery
Recovery is usually smooth and includes:
- Hospital stay of 1–2 days
- Gradual return to oral liquids within 24 hours
- Soft diet for a few weeks
- Return to normal activities in 1–2 weeks
- Significant improvement in swallowing
Possible Risks and Complications
Although the surgery is safe, possible risks include:
- Bleeding
- Infection
- Acid reflux
- Difficulty swallowing (temporary)
- Esophageal perforation (rare)
- Recurrence of symptoms
Choosing an experienced surgeon greatly reduces these risks.
Life After Achalasia Surgery
Most patients experience dramatic improvement in swallowing and quality of life. Long-term follow-up and lifestyle adjustments such as eating slowly, chewing well, and maintaining a healthy weight help ensure lasting benefits.
When to Consult a Doctor
Contact Us if you experience:
- Persistent difficulty swallowing
- Severe chest pain
- Fever or signs of infection
- Vomiting or inability to eat
