Rectal prolapse is a medical condition in which the rectum (the last part of the large intestine) slips down and protrudes through the anus. This condition can cause discomfort, embarrassment, and difficulty with bowel movements. Rectal prolapse is more common in older adults but can affect people of all ages, including children. With early diagnosis and proper treatment, most patients can achieve good symptom control and improved quality of life.
This article explains everything a patient needs to know about rectal prolapse, including causes, symptoms, types, diagnosis, treatment options, recovery, and prevention.
What Is Rectal Prolapse?
The rectum is normally supported by muscles and ligaments in the pelvis. When these supporting structures weaken, the rectum may slide out of its normal position and protrude through the anal opening. Rectal prolapse may occur during bowel movements or remain outside the anus permanently in severe cases.
It is a progressive condition, meaning it tends to worsen over time if left untreated.
Types of Rectal Prolapse
Rectal prolapse is classified into three main types:
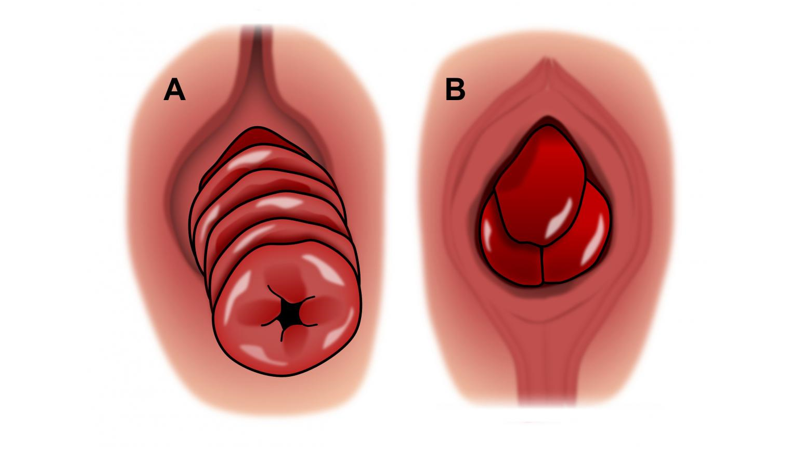
1. Partial (Mucosal) Prolapse
Only the inner lining of the rectum protrudes through the anus. This is often seen in children and mild cases.
2. Complete (Full-Thickness) Prolapse
The entire wall of the rectum comes out through the anus. This is the most common and severe form.
3. Internal Prolapse (Intussusception)
The rectum folds into itself but does not come out of the anus. It may cause symptoms of constipation and incomplete bowel emptying.
Causes and Risk Factors
Several factors can contribute to rectal prolapse, including:
- Chronic constipation and straining
- Long-term diarrhea
- Weak pelvic floor muscles
- Aging
- Pregnancy and childbirth
- Neurological disorders
- Previous pelvic or anorectal surgery
- Chronic coughing
- Poor muscle tone in the rectum
- Malnutrition
In children, rectal prolapse may be associated with malnutrition, diarrhea, or parasitic infections.
Symptoms of Rectal Prolapse
Common symptoms include:
- A red or pink mass protruding from the anus
- Feeling of something "coming out" during bowel movements
- Difficulty controlling bowel movements
- Constipation or diarrhea
- Mucus or blood discharge
- Anal discomfort or pain
- Feeling of incomplete bowel emptying
- Irritation or itching around the anus
Symptoms often worsen with time and physical strain.
How Is Rectal Prolapse Diagnosed?
Diagnosis is usually based on medical history and physical examination. Additional tests may include:
- Colonoscopy or sigmoidoscopy
- Defecography
- MRI or CT scan
- Anal manometry
- Ultrasound
These tests help identify the type of prolapse and rule out other conditions.
Treatment Options for Rectal Prolapse
Non-Surgical Treatment
In non-surgical treatment options, mention about the pelvic floor muscles, strengthening exercises which are also called as a Keigel’s exercises. These are very important and crucial for the strengthening of the pelvic floor muscles and preventing or increasing mild rectal prolapse into the full thickness and complications.
Surgical Treatment
Surgery is the most effective treatment for rectal prolapse, especially for complete or recurrent cases. The choice of surgery depends on the patient's age, overall health, and severity of prolapse.
Abdominal Procedures
- Rectopexy (fixing the rectum to the sacrum)
- Laparoscopic or robotic rectopexy
- Resection rectopexy (removal of part of the colon)
These procedures have lower recurrence rates and are preferred for fit patients.
Perineal Procedures
- Delorme's procedure
- Altemeier's procedure (perineal rectosigmoidectomy)
These are suitable for elderly or high-risk patients.
Benefits of Laparoscopic Surgery
Minimally invasive (laparoscopic) surgery offers several advantages:
- Smaller incisions
- Less pain
- Reduced hospital stay
- Faster recovery
- Lower risk of infection
- Better cosmetic results
Many rectal prolapse surgeries are now performed laparoscopically.
Recovery After Rectal Prolapse Surgery
Recovery varies depending on the type of surgery. Most patients can expect:
- Hospital stay of 2–5 days
- Gradual return to normal diet
- Avoiding heavy lifting for several weeks
- Improved bowel control over time
- Follow-up visits with the surgeon
Complete recovery may take several weeks.
Possible Risks and Complications
As with any surgery, rectal prolapse surgery carries some risks:
- Infection
- Bleeding
- Recurrence of prolapse
- Constipation or diarrhea
- Incontinence
- Injury to surrounding organs
Choosing an experienced surgeon reduces these risks.
Living with Rectal Prolapse
Early treatment can significantly improve quality of life. Lifestyle changes such as maintaining a healthy diet, managing bowel habits, and pelvic floor strengthening play an important role in long-term success.
When to See a Doctor
Seek medical attention if you notice:
- A protruding mass from the anus
- Persistent constipation or incontinence
- Pain or bleeding during bowel movements
- Worsening symptoms over time
Early diagnosis leads to better outcomes.
